A quiet epidemic is creeping across skin, homes, and entire healthcare systems — and almost no one is talking about it. More accurately, they’re talking around it: blaming eczema, mislabeling rashes, overprescribing steroids and anti-fungals, and dismissing persistent symptoms as psychosomatic. But what if what’s really behind these stubborn skin conditions isn’t eczema, fungal infections, or 'just dry skin'?
What if it’s mites…specifically Demodex and scabies.
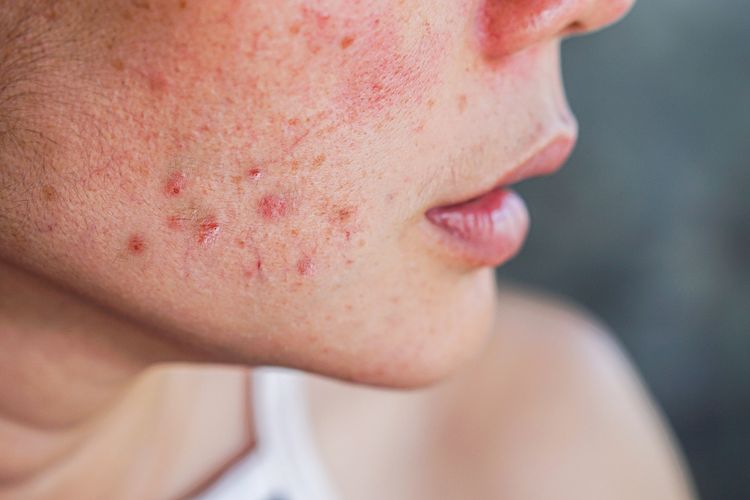
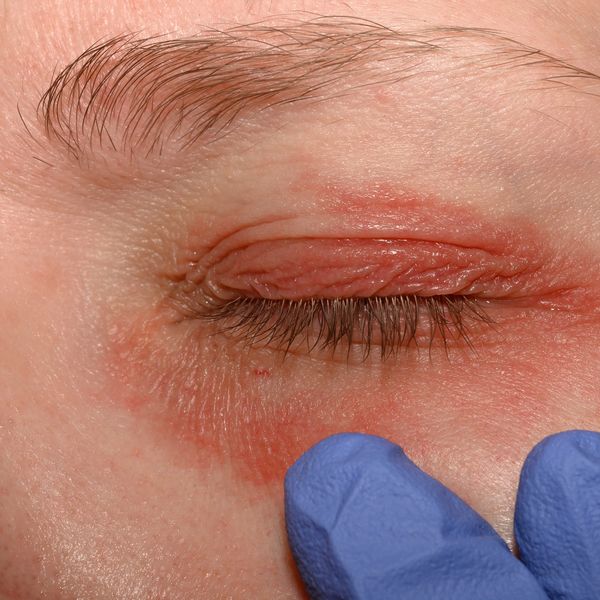
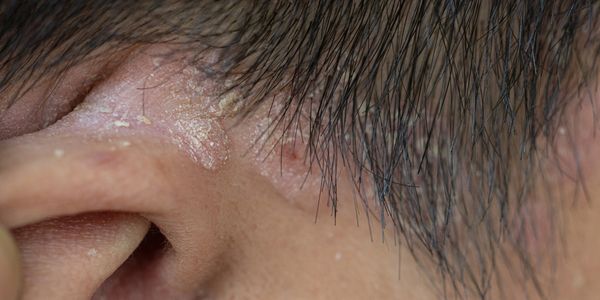
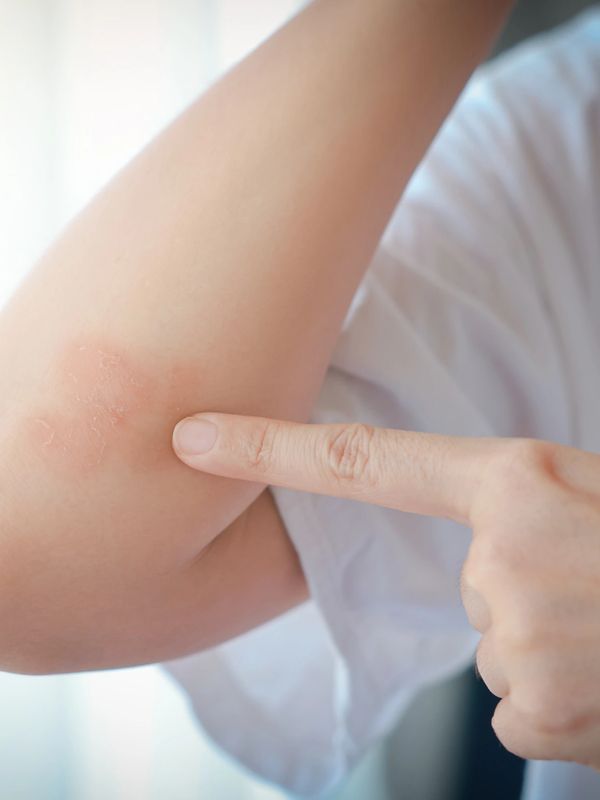
Demodex spp., follicle mites, are two different microorganisms that live in the hair follicles (D. folliculorum) and in the glands of the follicles on oily areas of the body (D. brevis). They are a normal aspect of a healthy skin barrier, but an overgrowth can produce signs and symptoms that mimic acne, eczema, psoriasis, contact dermatitis, allergic reactions and heat rash.
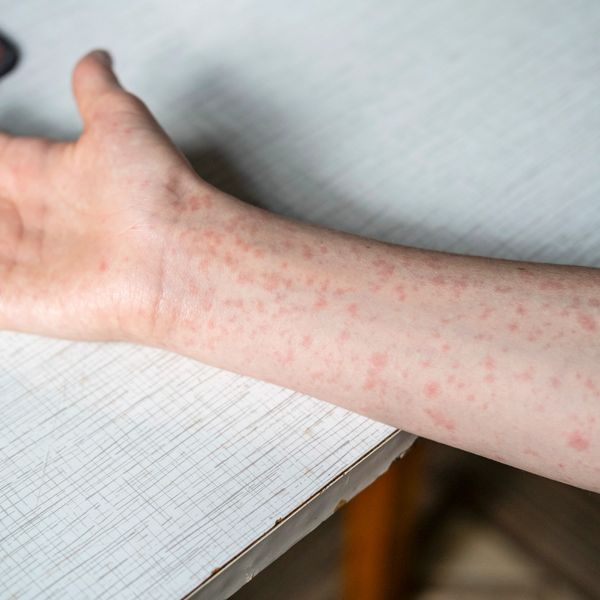
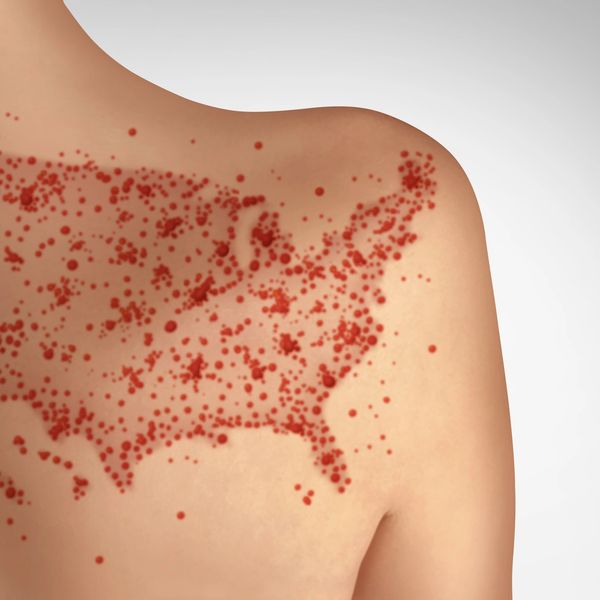
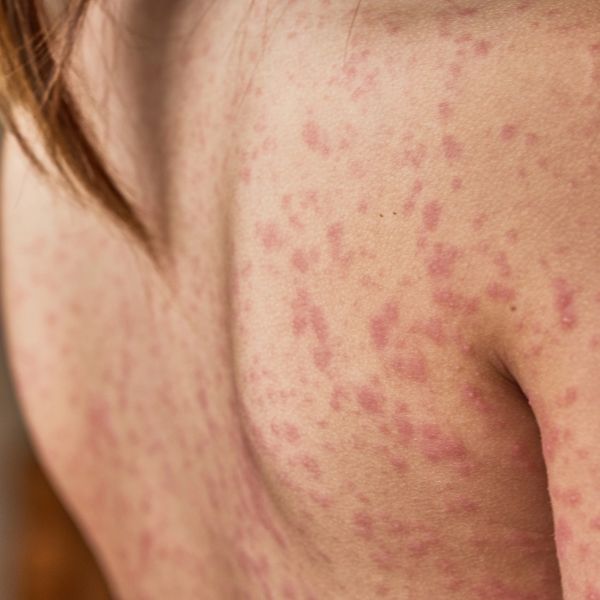
Sarcoptes scabiei, the human itch mite, burrows deep into the skin making tiny red dots or tunnels that appear on the surface as thin, sometimes silvery, lines or red scratches. Scabies mites and eggs are microscopic and almost impossible to see with the naked eye, but scabies mites leave tell tale trails and an intense itch, more so at night and early on in exposure. An infestation can cause immune responses and allergic reactions that not only mimic common skin conditions but also many autoimmune, mental health and neurological disorders.
Heavy metals in food, water, medications, personal products, and environmental exposure have created the perfect storm for ecto and endoparasites to thrive.